Getting paid for medical care sounds simple. A patient visits a clinic, a service takes place, and payment follows. Real life rarely works that way. Billing in health care includes many steps, many rules, and many chances for delay. This article explains how billing works, why errors happen, and what helps practices keep cash flow steady.
The goal is to give a plain-language view of a system that affects doctors, staff, and patients alike. You will see how claims move through the system, where problems show up, and what strong billing habits look like in daily practice.
The Story Behind a Medical Bill
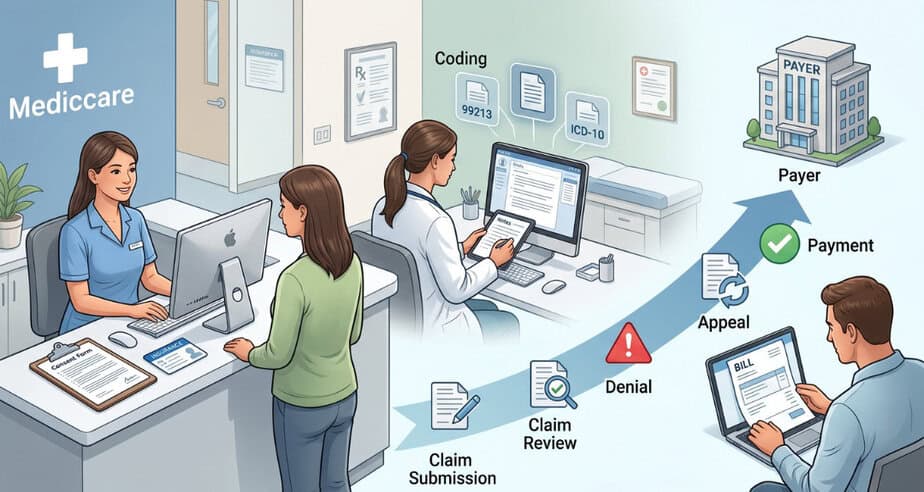
A medical bill starts at the front desk. Patient details, insurance data, and consent forms all feed the billing record. A single typo at this stage can follow the claim for weeks.
Next comes documentation. The clinician notes what care took place. These notes guide code selection. Codes are numbers that describe services in a standard way. Payers rely on them to decide payment.
After coding, a claim goes to an insurance company. The payer checks coverage, rules, and medical need. Payment, denial, or a request for more details follows. Each step has timelines set by contract or law.
Common Terms Explained in Plain Language
Billing has its own vocabulary. Knowing the basics helps non-experts follow along.
- Claim: A request for payment sent to a payer.
- Code: A number that stands for a service or diagnosis.
- Denial: A notice that a claim was not paid.
- Appeal: A request to review a denial.
- Patient balance: The part the patient owes after insurance.
These terms show up on statements and calls with insurers. Clear understanding reduces stress for staff and patients.
Why Errors Happen So Often
Health care billing touches clinical notes, software, contracts, and laws. Mistakes often come from gaps between these areas.
A study from the American Medical Association shows that claim denials affect a large share of practices each year. Many denials trace back to simple issues like missing data or expired coverage.
Staff turnover also plays a role. New team members need time to learn payer rules. Without clear guides, errors repeat.
Frequent Sources of Trouble
- Wrong or outdated insurance details
- Codes that do not match notes
- Missed filing deadlines
- Rules that vary by payer
Each item alone seems small. Together they slow down payment and raise costs.
The Human Side of Billing
Behind every claim sits a person. Front desk staff juggles phones and check-ins. Billers track hundreds of open claims. Clinicians balance care and charting.
One practice manager shared this view in a trade journal: “Billing stress rises when teams feel rushed. Time for checks saves time later.” That simple idea guides many strong offices.
Patients feel the impact too. Confusing bills lead to calls and worry. Clear statements and quick answers build trust.
Tools That Support Accuracy
Modern billing uses software, yet tools only help when used well. Systems pull data from charts and apply rules. They also flag missing items.
Below is a table showing common tools and what they handle.
| Tool Type | Main Role | Example Use |
| Practice system | Holds patient records | Demographics and notes |
| Coding aid | Suggests codes | Checks note details |
| Claim checker | Finds errors | Spots missing fields |
| Payment tracker | Follows payments | Flags delays
|
Training matters as much as the tool itself. A well-trained team spots issues before claims leave the office.
A Short Case Example
A mid-size clinic saw payments slow down over six months. Cash on hand dropped. Staff spent hours on calls.
A review showed that many claims lacked a referral number. The number was in the chart, yet not sent on the claim.
The fix was simple. The team added a checkpoint before submission. Within two months, denial rates fell. Payment speed improved.
This story shows how small process changes can make a real difference.
Outsourced Help and Internal Teams
Some practices handle billing in-house. Others work with outside groups. Each path has trade-offs.
Internal teams offer direct control and quick feedback. Outside groups bring scale and broad payer knowledge. Cost, staff size, and visit volume shape the choice.
When people talk about physician billing solutions, they often mean a mix of people, process, and tech working as one. You can read more context on this topic at physician billing solutions.
Measuring What Matters
Billing health shows up in numbers. Tracking them helps leaders spot issues early.
Common measures include:
- Days in accounts receivable
- Denial rate
- Clean claim rate
- Patient collection rate
The Medical Group Management Association publishes benchmarks each year. Comparing numbers against peers gives a useful perspective.
Ethics and Rules
Billing follows laws at the federal and state levels. These rules protect patients and public funds. They also guide fair payment.
Examples include coding standards and anti-fraud laws. Training on these topics protects practices from fines and audits.
Ethical billing also means clear communication. Patients deserve to know what they owe and why.
What Patients Can Do
Patients play a role in smooth billing. Simple steps help.
- Check insurance details each visit
- Ask for itemized statements
- Call early with questions
Many offices now offer online portals. These tools show balances and payment history in one place.
Where Billing Is Headed
Health care keeps changing. Value-based care ties payment to outcomes. This adds new data needs and reports.
Automation will keep growing. Even so, human review stays vital. Rules change often, and context matters.
Education will remain central. Teams that learn together adapt faster.
Final Thoughts and Next Steps
Medical billing links care and payment. It affects clinic health and patient trust. Clear steps, trained teams, and steady review form the base of strong performance.
Readers who want to learn more can explore reports from groups like the AMA and MGMA. These sources share data and guidance that support better billing habits.
Understanding the process brings calm to a topic that often feels stressful. With the right knowledge, billing becomes a managed task rather than a daily fire drill.
Read next: 10 Ways To Improve The Healthcare Quality In Hospitals
